Amethyst Piatra Neamt has officially opened its doors! Schedule an appointment
Amethyst Piatra Neamt has officially opened its doors! Schedule an appointment
History of radiotherapy
In 1896, a German-born physics professor, Wilhelm Conrad Roentgen, gave a remarkable lecture entitled “Considerations on a New Kind of Rays”. Roentgen called it “X-ray”, “x” being the algebraic symbol for the name of an unknown quantity. This work immediately created excitement around the world. Within months, systems were designed to use X-rays for diagnosis, and 3 years later radiation was being used to treat cancer.
In 1901, Roentgen received the first Nobel Prize in physics. Radiotherapy began with radium and low-voltage diagnostic machines. In France, a major breakthrough was made when it was discovered that giving daily doses of radiation over several weeks greatly improves a cancer patient’s chance of recovery. The methods and machines that deliver radiotherapy have improved steadily since then. Today, radiation is delivered with great precision to destroy cancerous tumours while limiting damage to surrounding normal tissues.
Many early-career radiologists used their own skin on their hands to test the irradiation power of radiotherapy machines, looking for a dose that could produce a pink reaction (erythema) that looked like sunburn. They called this the “erythemal dose” and the effect was thought to be a fair estimate of the daily fraction corresponding to the radiation.
In the early 1900s, radium was used as a source of radiation, and later, devices were developed using cobalt as a source of irradiation. This equipment was simple and produced cobalt 60 gamma rays. Since the 60s, most equipment using cobalt has been replaced by accelerators producing X-rays.
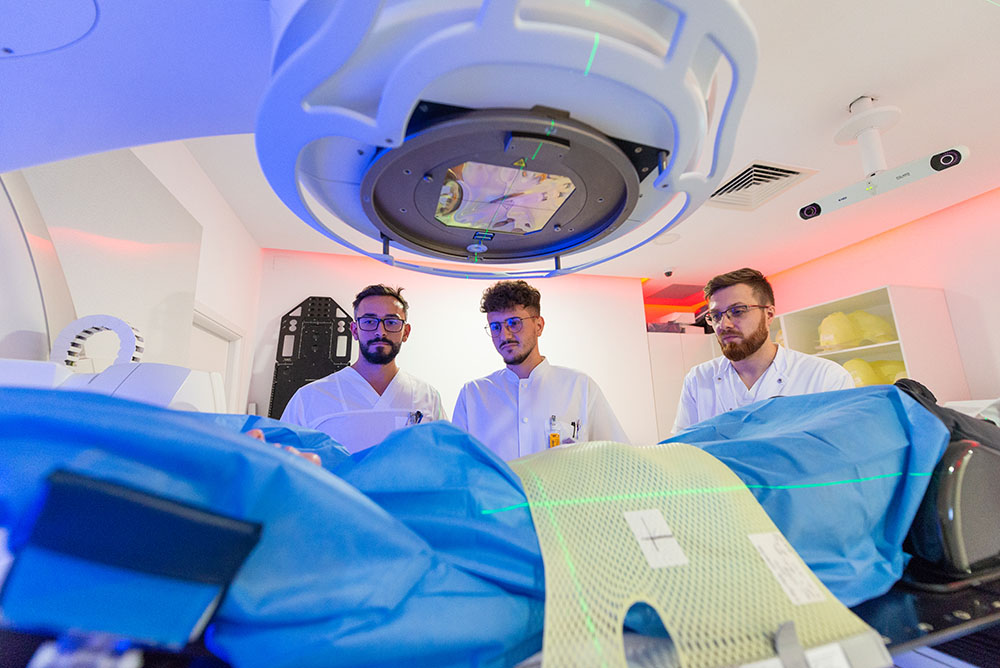
Modern radiotherapy
Advances in radiation physics and computer technology in the latter part of the 20th century made it possible to steer radiation more precisely. Conformal radiotherapy (CRT) uses CT images and special computers to map the location of a cancerous tumour very precisely in 3 dimensions. The patient may be immobilised with a plastic mask to keep the targeted body part in the same position for each treatment. The radiation beams are tailored to the shape of the tumour and aimed at it from several directions. Intensity-modulated radiation therapy (IMRT) is the same as CRT, but in addition to transmitting beams from several directions, their intensity (concentration) can be adjusted. This gives more control over the possibility of reducing the amount of radiation reaching healthy tissue while giving a high dose of radiation to cancer cells.
Stereotactic radiosurgery and stereotactic radiotherapy are terms that describe several techniques used to deliver a high, precise dose of radiation to a small tumour. Elekta’s linear accelerator, or other special machines such as the CyberKnife, are used to provide this type of treatment.
The year 1960 marked the beginning of widespread use of radiotherapy both in the United States and throughout Europe. This expansion has been largely due to the increasing availability of commercial linear accelerators and other equipment produced by active companies such as Elekta Limited that have developed treatment machines present in radiotherapy centres around the world to date.
In the years to come, the field of radiotherapy was to undergo several technological revolutions. Since the late 1980s, the use of computed tomography (CT) for treatment planning has become commonplace, and this has enabled the development of three-dimensional conformal radiotherapy (3D-CRT). 3D-CRT greatly improves the quality and effect of radiotherapy by reducing the dose delivered to surrounding healthy tissue.
IMRT treatment technique
The next major technological development known as Intensity Modulated Radiation Therapy (IMRT) is arguably the most important revolution in radiation oncology. Unlike conventional approaches, IMRT conforms the prescribed dose to the target area in 3 dimensions, thereby reducing the amount of healthy tissue receiving high doses of radiation and the risk of possible side effects.
IMRT is also a safety measure for making the decision to increase the prescribed medical dose and allows for retreatment of previously irradiated patients, improving the potential for cure.
While initially only available to a limited number of academic centres, IMRT technology has been rapidly adopted by the radiotherapy community in recent years. A 2005 study showed that nearly 75% of radiation therapists in the United States treat patients using IMRT. This was all the more remarkable given that earlier, in the 2003 survey, less than a third of radiotherapists were found to be using IMRT.
The latest innovation in IMRT is the rotational approach, which involves a rotating motion of the accelerator around the patient to target radiation at the diseased tissue from different angles. Modulation is created by overlapping arcs. First described in 1995 as “Intensity Modulated Arc Therapy” by Dr. Cedric Yu, since the 2000s it has been known as Volumetric Arcterapy.
Today, radiotherapy researchers are working on future equipment that will incorporate IGRT (image-guided radiotherapy). IGRT is rapidly growing in popularity, primarily due to the widespread adoption of new linear accelerators, which function as both treatment and imaging devices.
This new function will allow future treatment to be adapted to changes in the tumour. The scientific world is currently actively investigating the potential roles of IGRT in a large number of tumour sites to achieve higher cure rates and lower toxicity rates.
Radiotherapy in Amethyst clinics
The ELEKTA accelerator available in Amethyst Radiotherapy Centres has 2 unique functions in Romania:
Phone: 021.9368
Address: no 42, Drumul Odăii, Otopeni, Ilfov County
Phone: 021.9368
Address: no 486G, Răzoare Street, Florești, Cluj County
Phone: 021.9368
Address: no 12, Bela Bartok Street, Dumbrăvița, Timiș County
Phone: 021.9368
Address: no 10, Louis Pasteur Street, Alba-Iulia, Alba County
Phone: 021.9368
Address: no 31H, Ion Ionescu de la Brad, Piatra Neamț, Neamț County
Phone: 021.9368
Address: no 9, Dunării Street, Satu Mare, Satu Mare County